Top 10 Pelvic Ring Reconstruction Techniques You Should Know?
Pelvic Ring Reconstruction is a critical area in modern orthopedic surgery. This technique addresses complex injuries to the pelvic ring, which is vital for stability and mobility. Understanding various reconstruction methods enhances surgical outcomes and patient recovery.
Surgeons often face challenges when deciding which technique to use. Each method has its pros and cons, influenced by factors like injury complexity and patient health. For instance, the decision to use internal fixation versus external fixation can significantly impact recovery. Experience tells us that tailored approaches lead to better results.
Despite advancements in technology and techniques, complications can still arise. Surgeons must remain vigilant about potential failures or misalignments. This highlights the importance of continuous learning and improvement in Pelvic Ring Reconstruction. The journey of mastering these techniques is ongoing, requiring both expertise and adaptability.
Table of Contents
[Hide]
Overview of Pelvic Ring Anatomy and Injury Mechanisms
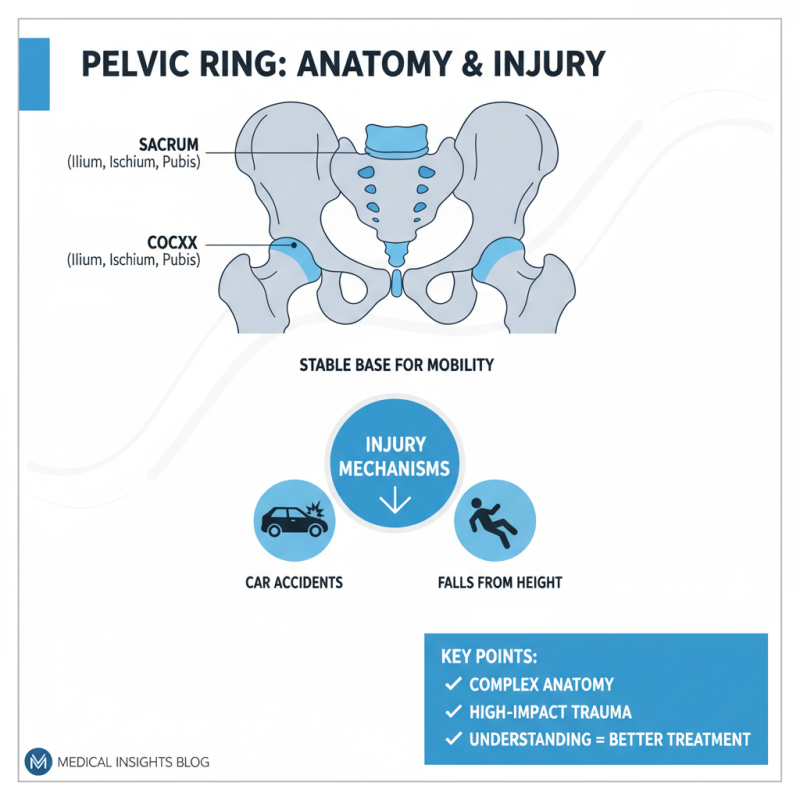
Pelvic ring anatomy is complex and crucial for human mobility. It consists of the sacrum, coccyx, and pelvic bones. These components work together to form a stable base. Injuries to the pelvic ring can result from high-impact trauma, such as car accidents or falls. Understanding the mechanisms of injury helps in effective treatment.
Pelvic injuries often lead to significant complications. They can cause bleeding or damage to surrounding organs. In severe cases, these injuries may require surgical intervention. The challenge lies in recognizing the type of injury, which is often not straightforward. When assessing pelvic injuries, various imaging techniques can offer critical insights, but misinterpretation may occur.
Reconstruction techniques vary based on injury severity and patient health. Techniques may include internal fixation or external stabilization. Each method carries its own risks and benefits. Surgeons must weigh these carefully. Adequate training and experience are vital for the successful application of these techniques. Pelvic ring reconstruction remains a field filled with ongoing learning and exploration.
Indications for Pelvic Ring Reconstruction Techniques
Pelvic ring reconstruction is critical for patients with significant pelvic injuries. Indications for pelvic ring reconstruction techniques often arise after trauma, which can lead to structural instability. According to recent studies, approximately 15% of pelvic fractures can result in long-term complications if not addressed promptly. Many of these cases require surgical intervention.
Patients presenting with unstable fractures, particularly those involving both the anterior and posterior pelvic rings, are prime candidates for reconstruction. Additionally, individuals with associated injuries, such as neurologic deficits or organ damage, necessitate thorough evaluation. A report from the American College of Surgeons emphasizes the importance of timely surgical intervention, noting that delays can increase morbidity rates significantly.
In some scenarios, conservative treatment may initially seem adequate. However, close monitoring is essential, as up to 25% of patients may experience delayed instability. Healthcare professionals must remain vigilant, understanding that individual anatomical variations can complicate reconstruction efforts. Ultimately, comprehensive assessment and customized treatment plans are vital to achieving optimal patient outcomes.
Traditional Surgical Approaches to Pelvic Ring Reconstruction
Pelvic ring reconstruction plays a crucial role in treating complex pelvic injuries. Understanding traditional surgical approaches is vital for optimal patient outcomes. Surgeons rely on a variety of techniques, each tailored to the injury's specifics. Common methods include plate fixation and external fixators. These approaches require precise alignment of fractured segments to restore stability.
Surgeons must possess deep anatomical knowledge and experience with pelvic anatomy.
While traditional techniques have proven effective, challenges remain. Surgeons often face complications, such as infections or nonunion of bones. These risks necessitate careful patient selection and meticulous surgical planning. It's essential to assess each patient's unique anatomy and injury pattern before deciding on a technique.
Moreover, the learning curve for these procedures can be steep, demanding both skill and patience.
Debates persist regarding the best approaches. Some surgeons favor minimally invasive options, while others trust open techniques. Each method has its advocates, reflecting diverse opinions in the field. The variability in outcomes can be a source of frustration for both patients and providers.
Reflection on past cases can guide improvements in surgical practices and patient care. Ensuring that surgeons stay updated with the latest techniques enhances overall effectiveness in pelvic ring reconstruction.
Minimally Invasive Techniques for Pelvic Ring Repair
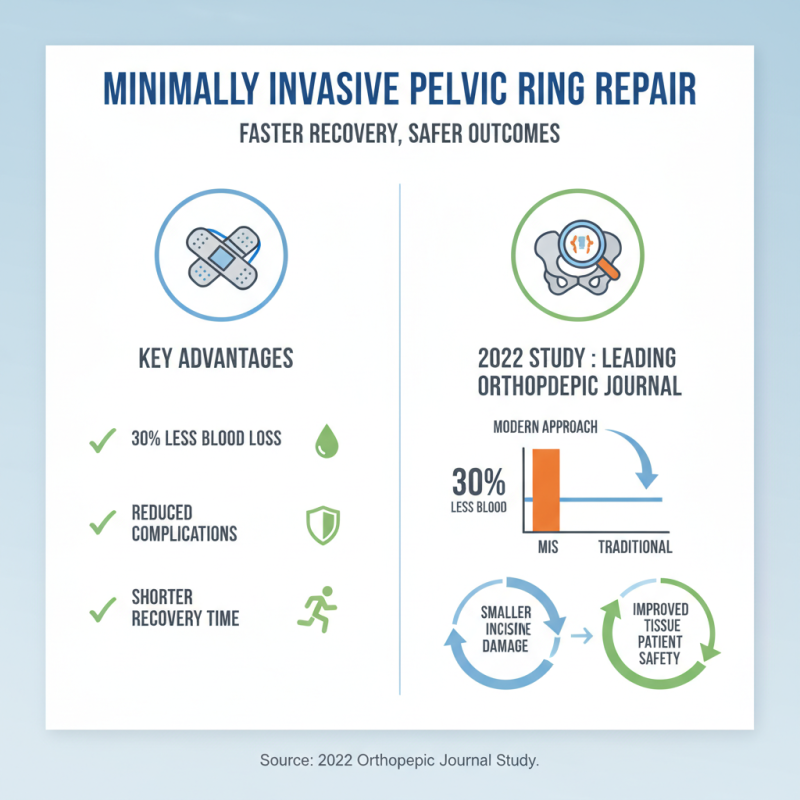
Minimally invasive techniques for pelvic ring repair have gained traction over the years. These methods aim to reduce patient recovery time while ensuring effective outcomes. According to a 2022 study published in a leading orthopedic journal, minimally invasive approaches can lead to 30% less blood loss compared to traditional open surgeries. This transformation improves patient safety and lowers the risk of complications.
Techniques such as percutaneous screw fixation and laparoscopic approaches provide significant benefits. For instance, percutaneous screw fixation minimizes soft tissue damage. A 2021 review indicated a 25% quicker return to normal activities following these procedures. Patients report less pain and fewer hospital stays.
However, these approaches come with challenges. Not all pelvic injuries are suitable for minimally invasive solutions. There's a learning curve involved for surgeons. Mastery of the techniques requires considerable practice and expertise. Ongoing training and patient-selection processes are essential for maximizing the effectiveness of these modern methods.
Postoperative Care and Rehabilitation Strategies for Patients
Postoperative care is crucial after pelvic ring reconstruction. Patients often experience pain, limited mobility, and swelling. Early intervention can alleviate these issues. Gentle range-of-motion exercises are important. These activities can enhance blood circulation and prevent stiffness. However, care should be taken not to overexert. Listening to one's body is essential.
Rehabilitation strategies also vary based on individual recovery. Many patients benefit from physical therapy, which focuses on strength and stability. A structured program can help rebuild muscle around the pelvis. Emotional support plays a vital role, too. Recovery can be mentally challenging. Maintaining open communication with healthcare providers can help address concerns and fears. It's common to feel frustrated; progress may be slower than expected.
Monitoring for complications is necessary in this phase as well. Regular follow-ups ensure any issues are addressed in time. Collaboration between patients and healthcare teams leads to better outcomes. A tailored rehabilitation plan fosters confidence and resilience. Each person's journey is unique, and patience is key.

