10 Essential Tips for Choosing Bone Graft Substitutes for Successful Surgery?
When considering surgical procedures involving bone grafts, the choice of Bone Graft Substitutes becomes crucial. These substitutes can significantly impact the success of the surgery and the recovery process. Surgeons must evaluate several factors, including the specific needs of the patient, the type of surgery, and the material properties of the substitutes available. Each option has unique advantages and potential drawbacks that should not be overlooked.
Selecting the right Bone Graft Substitute requires a balance of expertise and insight. It is essential to review clinical studies and guidelines to understand the effectiveness of different materials. Some substitutes may offer rapid integration, while others may pose risks of complications. Every surgical team should weigh these aspects carefully, contemplating past experiences and outcomes.
In an evolving field, staying informed about the latest developments is vital. Each choice made in the operating room informs future decisions, contributing to a cycle of learning and adaptation. Surgeons should embrace a reflective mindset, questioning their choices and remaining open to new evidence. The right Bone Graft Substitute not only fosters healing but also builds a foundation for ongoing surgical excellence.
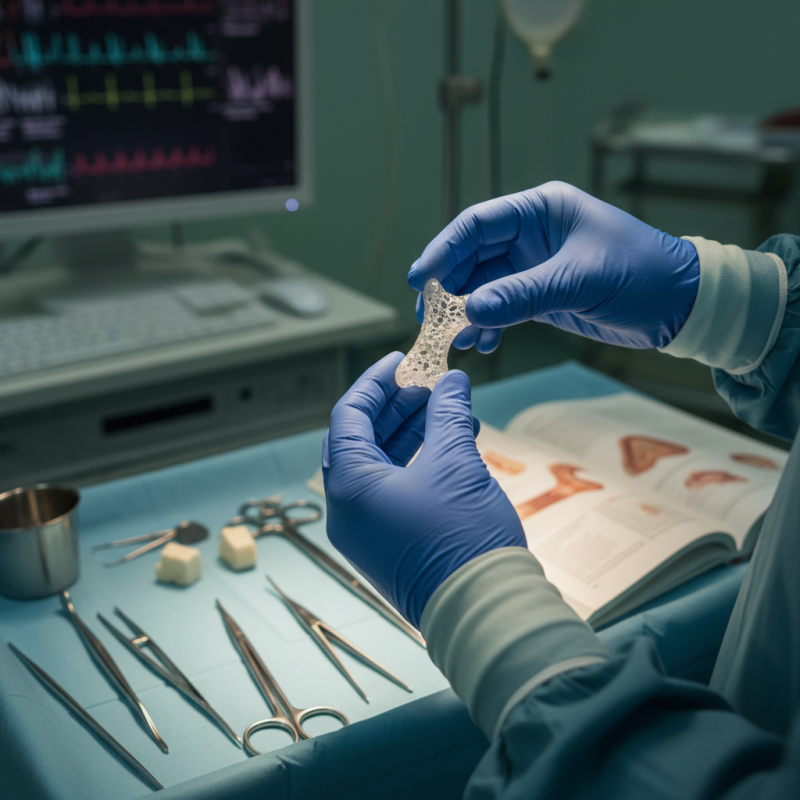
Table of Contents
[Hide]
Understanding Bone Graft Substitutes: An Overview of Options
Bone graft substitutes are vital in orthopedic and dental surgeries. These materials support bone regeneration, especially when natural grafts are not feasible. A study by the Journal of Bone and Joint Surgery highlights that around 50% of bone graft procedures use synthetic or allograft substitutes. This shift reflects surgeons' need for reliable options that promote healing and minimize donor site morbidity.
Several options exist, including ceramics, polymers, and composites. Hydroxyapatite is a popular choice due to its excellent biocompatibility. Research indicates a higher success rate with ceramics in spinal fusion surgeries. However, not all substitutes promote vascularization effectively, leading to slower integration with host bone. A report from the International Journal of Oral & Maxillofacial Surgery mentions that some substitutes fail to achieve desired mechanical properties, which can impact the overall healing process.
It’s essential to understand the biological environment when selecting graft substitutes. Surgeons must consider factors like porosity and resorption rates. Some substitutes may not perform well under specific conditions, raising concerns about long-term stability. Data from clinical trials show discrepancies in outcomes, emphasizing the need for more research. As options continue to evolve, ongoing evaluation of these materials is necessary to ensure positive surgical results.
Bone Graft Substitute Options and Their Success Rates
This chart illustrates the success rates of various bone graft substitutes commonly used in surgeries. As shown, different materials exhibit varying levels of efficacy.
Key Factors to Consider When Selecting a Bone Graft Substitute
Choosing the right bone graft substitute can significantly influence surgical outcomes. It is crucial to consider several key factors. One essential aspect is biocompatibility. The substitute should interact well with the body without provoking an adverse reaction. According to a report by the American Academy of Orthopaedic Surgeons, a well-chosen graft can enhance bone regeneration by up to 80%.
Another factor to ponder is the mechanical properties of the substitute. The substitute must withstand the stresses of the surgical environment. A recent study highlighted the importance of tensile strength and stiffness. Poor mechanical properties can lead to complications, such as failure at the graft site.
When evaluating options, consider these tips:
- Research the material's history and success rates. Knowing past performance provides insight into its reliability.
- Assess the support available post-surgery. A robust follow-up program can significantly impact recovery times.
- Seek opinions from experienced surgeons who have encountered various grafts. Their insights can reveal significant differences among substitutes.
While many substitutes exist, reflecting on these factors can guide better decision-making. No material is flawless, and understanding weaknesses is part of the selection process.
Evaluating Biocompatibility and Safety of Bone Graft Materials
When evaluating the biocompatibility and safety of bone graft materials, several factors come into play. The biological response is crucial. A material must not provoke an adverse reaction. Testing for biocompatibility often involves assessing how the material interacts with living tissue.
Tips for ensuring effective material selection include examining the source of the graft. Some options may have natural origins, while others are synthetic. Research shows that autografts usually lead to less rejection. However, the recovery time increases. It's essential to consider the trade-off between immediate recovery and long-term success.
Another critical factor is the physical properties of the graft substitute. The ideal material should have adequate porosity to promote cell infiltration. Low porosity can hinder successful bone regeneration. Be wary of products that lack transparent studies on their performance. It reveals the importance of rigorous clinical trials.
Ultimately, knowing the risk-benefit ratio is vital. While many materials can be effective, individual patient needs can differ significantly. Engage with healthcare professionals who can provide insights based on case studies and current research. Balancing safety, functionality, and patient-specific factors will lead to successful outcomes in bone grafting surgeries.
10 Essential Tips for Choosing Bone Graft Substitutes for Successful Surgery
| Tip No. | Tip | Biocompatibility | Safety Profile | Recommended Use Cases |
|---|---|---|---|---|
| 1 | Evaluate Material Composition | High | Low Risk | Dental Implants |
| 2 | Check for FDA Approval | Moderate | Moderate Risk | Spinal Fusion |
| 3 | Consider Handling Properties | High | Low Risk | Orthopedic Surgery |
| 4 | Evaluate Resorption Rate | Moderate | Moderate Risk | Fracture Repair |
| 5 | Assess Osteoconductivity | High | Low Risk | Bone Defects |
| 6 | Research Clinical Outcomes | Variable | Variable Risk | Revision Surgeries |
| 7 | Evaluate Cost-Effectiveness | N/A | N/A | General Use |
| 8 | Discuss with Peers | N/A | N/A | All Surgical Areas |
| 9 | Consider Surgical Technique Compatibility | High | Low Risk | Complex Procedures |
| 10 | Monitor Post-Operative Results | High | Low Risk | Long-Term Follow-Up |
Assessing the Growth and Healing Potential of Substitutes
When considering bone graft substitutes, assessing their growth and healing potential is crucial. Not all substitutes are created equal, and their biological compatibility plays a significant role in postoperative success. Look into the properties of each substitute. Some demonstrate better osteoconductive and osteoinductive capabilities, which are essential for bone regeneration.
Research has shown that some substitutes facilitate cellular attachment and proliferation better than others. Cellular behavior can vary widely, and understanding these differences is vital. Experimentation might reveal surprising results. For instance, a substitute that appears ideal in theory may not perform well in practice. Always consult peer-reviewed studies to ensure your choices are based on solid research.
Don’t overlook biomechanical properties. The stress and strain that a graft will endure can affect healing. Substitutes that deform under stress might lead to complications. It's an ongoing challenge in the field to align with the best practices while adapting to new materials and techniques. Continual learning and critical assessment of outcomes are necessary for fostering success in bone grafting procedures.
Cost Considerations and Availability in Bone Graft Selection
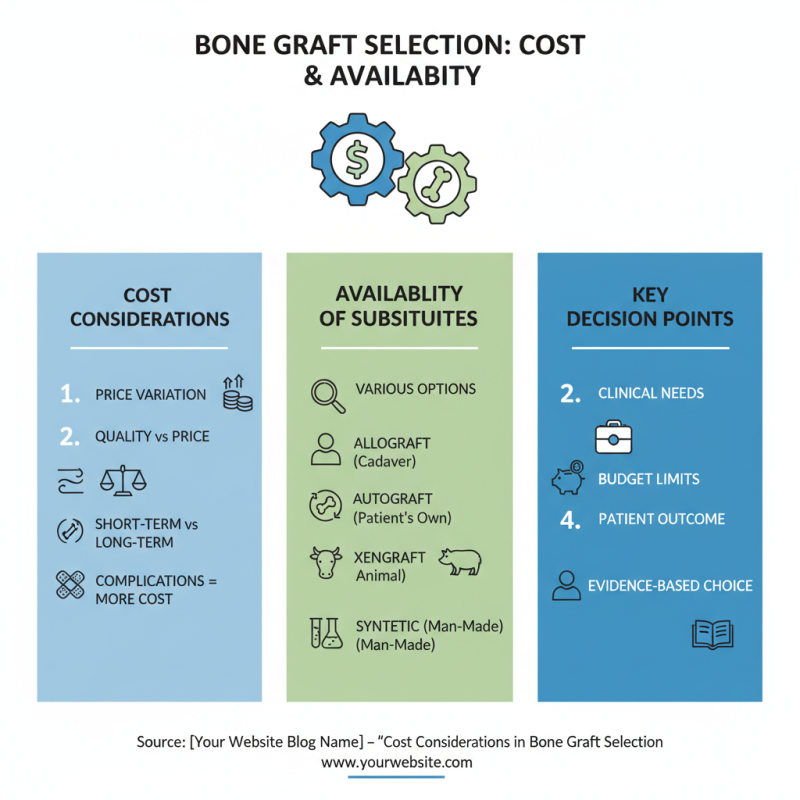
When choosing bone graft substitutes, cost is a significant factor. Various substitutes are available, but their prices can differ widely. It’s essential to compare costs while considering the quality. Some low-cost options may not provide the same benefits, leading to complications. Surgeons must evaluate the long-term costs versus short-term savings. Understanding the implications of these choices can prevent issues down the line.
Availability is another critical consideration. Some substitutes may not be readily accessible in specific regions. This can impact the surgical schedule and patient outcomes. Surgeons should develop relationships with suppliers to ensure they have a reliable source. Sometimes, alternatives may require additional effort to source, impacting the decision-making process.
In addition to these factors, healthcare professionals need to weigh the clinical evidence behind each option. Not all substitutes are created equal. Some may have limited research backing their effectiveness. It is vital to consider the existing studies and guidelines. This can guide healthcare providers to select the most appropriate solution for their patients. Balancing cost, availability, and clinical evidence is key in bone graft selection.
Related Posts
-

Top 10 Bone Graft Substitutes You Need to Know About?
-

How to Prepare for Limb Lengthening Surgery in 2026?
-
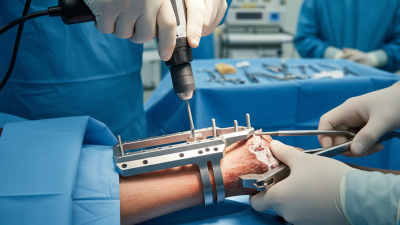
2026 How to Use a Distal Femoral Plate for Effective Fracture Treatment?
-
Why You Should Understand Intertrochanteric Femoral Fracture Risks?
-
What is Tibial Intramedullary Nail and How Does It Work?
-
Top 10 Pelvic Ring Reconstruction Techniques You Should Know?
